Several vein conditions affect the legs. Some vein conditions cause only cosmetic concerns, while others may indicate a more serious vascular disorder.
Varicose to Perfect provides comprehensive vein treatment. Our clinic in Springboro, Ohio, serves patients throughout the Cincinnati-Dayton area. Board-certified physician Dr. Sukir Sinnathamby, an interventional vascular specialist, leads our team.
If you have leg pain, restless legs, varicose veins, or spider veins, contact us to schedule a consultation. We will begin with a comprehensive evaluation and screening. Once we diagnose your condition, Dr. Sinnathamby will recommend the treatment options that are best for you.
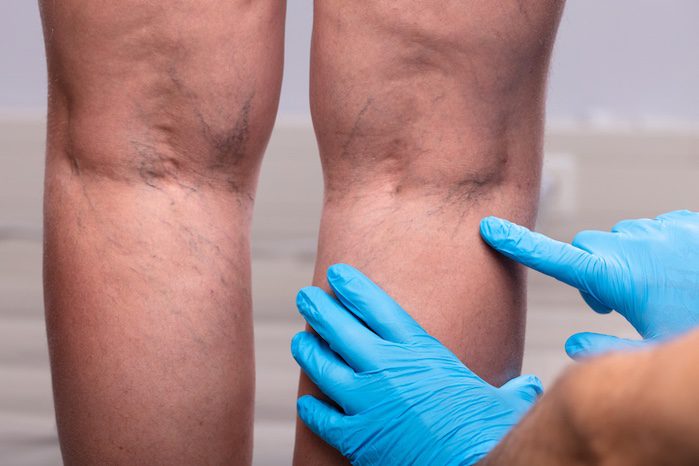
Common Leg Vein Conditions We Can Address
We can treat multiple types of common leg vein conditions in our office.
Spider Veins
Spider veins are a common and mild vein problem. While they’re typically not a health risk, most patients choose to remove them because they are unsightly.
Our spider vein treatments are minimally invasive and highly effective. Most spider vein treatments are pain-free and let you get back to your daily activities immediately. Two of the most common treatments for spider vein removal are:
- Vein Gough: A gentle, non-invasive technology that treats veins beneath the skin. It uses precise energy to close the vein, leaving your skin untouched.
- Sclerotherapy: A treatment that involves a direct injection that causes spider veins to collapse and fade from view.
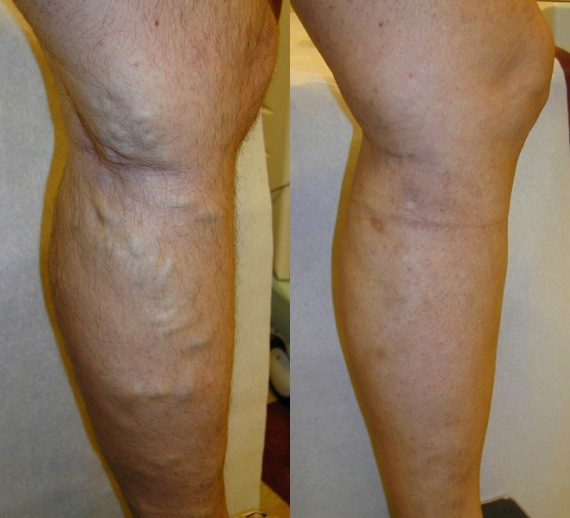
Varicose Veins
Varicose vein conditions can range from minor cosmetic concerns to more serious circulatory problems. Insurance covers most varicose vein treatments. Our team will guide you through the billing and help get pre-approval for your care.
We offer several minimally invasive treatments for varicose veins at our Springboro treatment center. These include Vein Gough, Laser Treatments, Ambulatory Hook Phlebectomy, and Sclerotherapy.
Faulty valves in your veins can cause blood to pool. This makes the veins swell and become visible bulges. Varicose veins can cause many painful symptoms, including:
- Leg pain
- Fatigue
- Heaviness
- Swelling
- Cramping
- Tingling, itching, or burning sensation
- Changes in skin color (darkening)
- Restlessness
Leg Ulcers
Venous leg ulcers, the most common skin ulcer, typically form just above the ankle. They are caused by poor circulation and high blood pressure in the lower leg veins. Although both men and women can develop them, these ulcers are most frequent in older women.
Warning signs and symptoms of leg ulcers include:
- Swelling
- Dry red skin
- Burning or itching sensations
- Raw/weeping wounds
In many cases, leg ulcers develop from poorly cared-for or untreated varicose veins. However, they can also develop as a result of blood clots, multiple pregnancies, obesity, or prolonged periods of standing.
There are several ways to treat this. One option is compression bandages. These special bandages squeeze the leg to reduce swelling and help blood flow.
The Causes of Leg Vein Conditions
Leg vein conditions occur when the veins in your legs do not work properly. Several factors, including genetics, lifestyle, and health conditions, can lead to these issues.
Genetics and Family History
One of the most common causes of leg vein conditions is genetics. Varicose and spider veins are often hereditary. This means that if your family members have them, you are more likely to develop them. Genetic factors can affect the strength of your vein walls and valves, increasing their likelihood of failure.
Aging
As people age, their veins naturally weaken. Over time, the valves in their veins can lose their ability to close tightly, allowing blood to flow backward and pool in them. As you age, your vein walls can weaken and stretch. This can lead to problems like varicose veins or chronic venous insufficiency (CVI).
Prolonged Standing or Sitting
Spending long hours on your feet or sitting can put extra pressure on your leg veins. Jobs that require standing, such as teaching, nursing, or retail work, can increase the risk of vein problems. Prolonged sitting slows blood flow in your legs, increasing the risk of vein conditions and blood clots. This is a key risk during long flights or while working a desk job.
Pregnancy
Pregnancy is another common cause of leg vein problems. During pregnancy, a woman’s body produces more blood to support the growing baby. This extra blood flow, combined with hormonal changes that relax vein walls, can strain the veins.
The baby’s weight also adds pressure to the veins in the pelvis and legs. Varicose veins often appear during pregnancy but may improve after delivery.
Obesity
Carrying extra weight puts additional pressure on the veins in your legs. This pressure can weaken vein walls and valves, making it harder for blood to flow upward to the heart. Obesity is a major risk factor for both varicose veins and chronic venous insufficiency.
Injuries or Surgery
Previous leg injuries, surgeries, or blood clots can damage the valves and walls of your veins. For example, deep vein thrombosis (DVT), which occurs when a blood clot forms in a deep vein, can lead to long-term damage. This damage often results in chronic venous insufficiency or post-thrombotic syndrome.
Hormonal Changes
Hormones can also play a role in vein conditions. Women are more likely than men to develop vein problems because of hormonal changes during puberty, pregnancy, and menopause. Birth control pills and hormone replacement therapy can also increase the risk.
Diagnosing Leg Vein Problems
Diagnosing leg vein conditions is important in understanding and treating problems that affect your veins. Your doctor will identify the cause of symptoms like swelling, pain, or visible veins. They do this through a physical exam, by reviewing your history, and with diagnostic tests. Early diagnosis can prevent serious complications and help you manage your condition effectively.
Medical History
The first step in diagnosing leg vein conditions is discussing your medical history. Your doctor will talk with you about your symptoms. You’ll discuss when they began and whether standing, sitting, or activity makes them feel worse.
They may also ask if you have a family history of vein problems, such as varicose veins or deep vein thrombosis (DVT). Sharing details about your lifestyle, medications, and previous injuries or surgeries helps the doctor identify possible causes.
Physical Exam
A physical exam helps the doctor look for visible signs of vein problems. They will examine your legs for swelling, discoloration, and bulging veins. We may ask you to stand during the exam so the doctor can check how gravity affects your veins. If you have symptoms like open sores or ulcers, the doctor will assess their size, location, and severity.
Duplex Ultrasound
A duplex ultrasound is one of the most common tests for diagnosing vascular conditions. This noninvasive test uses sound waves to create images of your veins and show how blood flows.
It helps doctors see whether your veins have blockages, clots, or valve problems. A technician moves a small transducer device over your skin during the procedure. The ultrasound provides real-time images that help pinpoint the issue.
Venography
Doctors sometimes use venography to get a clearer picture of your veins. This test involves injecting a contrast dye into your veins, which makes them visible on X-rays. Venography is especially useful for detecting deep vein thrombosis and other deep vein abnormalities. While less common than ultrasound, it can be valuable in complex cases.
Blood Tests
If the doctor suspects a blood clot or clotting disorder, blood tests may be ordered. These tests can measure D-dimer levels, a substance released when blood clots dissolve. High D-dimer levels may indicate the presence of a clot, prompting further investigation. Blood tests also help rule out other conditions that could mimic vein problems.
CT or MRI Scans
For more detailed imaging, doctors may use CT (computed tomography) or MRI (magnetic resonance imaging) scans. These advanced tests provide a 3D view of your veins and surrounding tissues. We often use these in complex cases or when other tests do not provide sufficient information.
Self-Monitoring and Reporting
You play an important role in diagnosing vein conditions by paying attention to your symptoms. Keep track of any swelling, pain, or changes in your legs, and share this information with your doctor. Even subtle symptoms, such as heaviness or fatigue in your legs, can provide valuable clues about your vein health.
Frequently Asked Questions
Learn more about leg vein conditions by reading the answers to these commonly asked questions.
Why do I suddenly have so many spider veins?
Several factors can cause sudden spider veins, including hormonal changes, prolonged standing, or a family history. Injuries, obesity, pregnancy, and too much sun exposure can cause them to appear more quickly in certain areas. If you notice a sudden increase in spider veins, contact your doctor to rule out underlying medical conditions.
Do spider veins mean diabetes?
No, spider veins are not a direct indicator of diabetes. However, in some cases, they can potentially be related. High blood glucose levels associated with diabetes can damage blood vessels. This can lead to vascular abnormalities.
However, many non-diabetic patients can develop spider veins due to genetics, hormone changes, or age. While diabetes can be a risk factor for some vascular diseases, it usually does not directly cause spider veins. Always consult a medical doctor for evaluation and proper diagnosis.
Do varicose veins ever go away?
Without treatment, varicose veins typically do not disappear on their own. In fact, they often gradually get worse over time. Varicosities rarely regress on their own.
However, early treatment can effectively block problem veins before they enlarge. Medications, compression stockings, and lifestyle changes can help you manage symptoms of visible varicose veins. Overall, the condition is unlikely to resolve without medical intervention.
What happens if you don’t remove varicose veins?
When you do not have a specialist remove your varicose veins, they could cause bleeding, blood clots, and leg ulcers. Moreover, over time, they might lead to pain and swelling in the legs. In more severe cases, varicose veins can lead to skin changes. There’s also a risk of developing non-healing sores and ulcers.
What happens if I don’t seek treatment for a venous ulcer?
If you do not seek treatment for venous leg ulcers, they will get worse. The ulcer may grow larger and deeper. Infection risk is also a significant concern.
It can spread to surrounding skin and even into your bloodstream. Moreover, the ulcer may continue to deepen, worsening the pain.
Leaving venous ulcers untreated can also lead to extreme pain and limb amputation. Early diagnosis and treatment are important to prevent progression.
What is the average healing time for a venous leg ulcer?
Most venous leg ulcers typically take 3 to 4 months to heal. However, some ulcers may take longer to heal. A small number of ulcers never heal.
The healing time for venous leg ulcers can vary depending on factors such as ulcer size. The underlying cause and the treatment’s effectiveness are also factors.
